A Healthier Future for West Virginia - Healthy People 2010
Federal 2010 Initiative
|
Contents Message Credits Introduction Objectives |
|
| 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 |
16 17 18 19 20 21 22 23 24 25 26 27 28 29 |

27 - Tobacco Use
Background
Tobacco
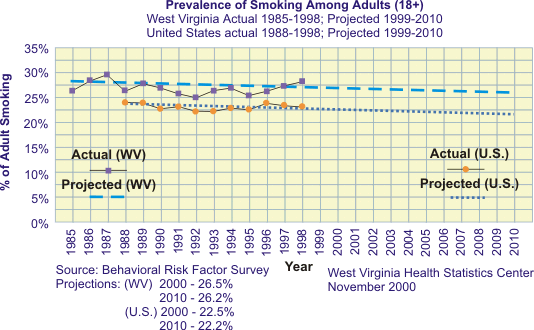
Tobacco use has plagued our society for hundreds of years and now has reached a public health crisis as the leading preventable cause of death and disease in the United States and in West Virginia. One in five deaths in our state is due to smoking, resulting in over 4,200 deaths in West Virginia each year and costing over $650 million annually. To put it in perspective, there are more deaths from smoking than deaths from alcohol, illegal drug use, suicide, homicide, AIDS, car accidents, and fires combined. Data from the 1998 Behavioral Risk Factor Surveillance System (BRFSS) survey indicated that West Virginia has a high rate of smoking (27.9%), ranking third in the U.S., with rates as high as 41% among lower-socioeconomic subpopulations.
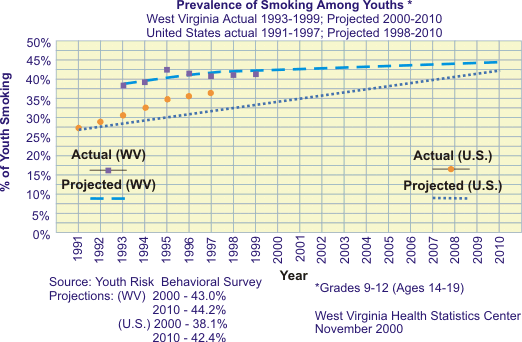
According to data from the 1999 Youth Risk Behavior Survey (YRBS), the rate of smoking among youths in grades 9-12 is 42.2%, fifth in the U.S. It is estimated that over 38,000 West Virginia kids now under the age of 18 will eventually die prematurely from tobacco-caused illness if current trends continue. About 80% of all smokers began cigarette use before they were 18. West Virginia youth have an average age of onset of smoking of between 13 and 14 years old. Cigarette smoking is associated with cancers of the lung, larynx, mouth, esophagus, bladder, kidney, pancreas, and cervix. It also causes chronic obstructive lung disease, including emphysema and chronic bronchitis, and heart disease and stroke. Other impacts of smoking are male impotence, exacerbation of asthma, increased risk of death from pneumonia and influenza, and wrinkles.
While the incidence of cigar smoking increased in our state during the 1990s, those using cigars and pipes remain relatively few in number compared to cigarettes and spit tobacco. Cigar use causes cancer of the larynx, mouth, esophagus, and lung.
According to vital statistics collected by the state, 25% of pregnant
women smoked during their pregnancies in 1998, and women of childbearing
age (18-34 years) smoked at a rate of about 35%. Smoking during pregnancy
can cause spontaneous abortion, low birthweight, premature birth, stillbirth,
and SIDS and increases the risk of birth defects. Female smokers also
may experience delayed
fertility and earlier menopause .
Secondhand smoke, or environmental tobacco smoke (ETS), causes lung cancer, heart disease, and increased asthma incidents in otherwise healthy nonsmokers. Children exposed to ETS may experience respiratory infections (middle ear infections, bronchitis, pneumonia) and asthma. The EPA has now classified ETS as a Class A carcinogen.
Smokeless Tobacco Use
West Virginia continues to rank first in the United States in the use of smokeless tobacco, or spit tobacco by adult men, with the 1998 BRFSS reporting a 17.5% rate of use. In 1999, about 28.6% of male youths used spit tobacco, a rank of third among YRBS survey states. While economic models do not include the cost to society of spit tobacco use, we know that users risk cancer of the mouth and nasal passages and tooth decay and gum disease.
The Tobacco Industry
While West Virginia was fortunate to be included in the National Cancer Institute's ASSIST Project, funding tobacco prevention from 1992 through1998, we have experienced very little decrease in the rates of smoking or spit tobacco use. The factor that most interferes with our success toward improved public health is the tobacco industry. Through 1998, the industry spent about $35 million each year in marketing its products in WV. This industry, more responsible than any other for negative public health, has engineered its products to contain higher concentrations of nicotine, influenced or suppressed medical research on tobacco, designed advertising geared toward youth, and legally challenged federal authority to regulate tobacco as a drug.
The tobacco settlement signed by 46 states including West Virginia in November 1998 is limited in restricting tobacco marketing. The settlement payments to West Virginia average about $60 million each year, but do not come close to the estimated $656 million annual cost of treating smoking-induced disease. In fiscal year 2001, $5.85 million will be spent on tobacco prevention. The U.S. Centers for Disease Control and Prevention (CDC) has recommended that West Virginia implement a tobacco prevention program that is funded at between $14 to $35 million annually.
Special Populations
Target populations for tobacco prevention include pregnant women, youth (including young adults up to 24 years), blue collar workers, and lower-socioeconomic groups. Minorities comprise about 4.3% of our state's population, 72% of whom are African American. We anticipate reaching this latter group through the faith community in selected cities and counties.
The Strategy
The Bureau's Tobacco Prevention Program, in cooperation with the Coalition for a Tobacco-Free WV and current local coalitions covering about 27 out of the 55 counties, will coordinate state and local projects in counter-marketing/media, communications, education, cessation, policy initiatives, and surveillance/evaluation. By far, policy change can have the greatest impact in creating and supporting the norm for a tobacco-free West Virginia.
Top of PageThe Objectives
FLAGSHIP OBJECTIVE
OBJECTIVE 27.1. Reduce the prevalence of cigarette smoking among youth
and adults.
27.1a. Reduce the prevalence of cigarette smoking among adults aged 18+
to 20% or lower. (Baseline: 28% in 1998)
27.1b. Reduce the prevalence of cigarette smoking among adults aged
18+ in the lower-socioeconomic level (12 years or less of education and
a household income of less than $25,000) to 25% or lower. (Baseline:
36% in 1998)
27.1c. Reduce the prevalence of cigarette smoking among women aged
18-24 (i.e., childbearing ages) to 25% or lower. (Baseline: 34.3%
in 1998)
27.1d. Reduce the proportion of youth in grades 6-12 who report smoking
in the previous month to 20% or lower. (Baseline: 42% in 1999)
Data Sources: West Virginia Bureau for Public Health (WVBPH), Office of Epidemiology and Health Promotion (OEHP), Behavioral Risk Factor Surveillance System (BRFSS); West Virginia Department of Education (WVDOE), Office of Healthy Schools (OHS), Youth Risk Behavior Survey (YRBS) and/or Youth Tobacco Survey (YTS)
On average, 12 West Virginians die every day because they smoked cigarettes.
Although their death certificates may list the cause of death as lung
cancer, heart disease, emphysema, or asthma, "cigarette smoking"
could just as well have been listed. The individuals who die from smoking-related
diseases come from all walks of life, all professions, all socioeconomic
groups, all family situations, all religions, and all ethnic backgrounds.
The loss of even one of these lives is immeasurable.
Every West Virginian, including those who have never smoked, pays $359
each year for the health care costs of smoking-related illness. This figure
does not include indirect costs such as forfeited earnings and lost productivity
due to illness and death, or health care and/or economic costs attributable
to snuff, chewing tobacco, cigars, pipes, and secondhand smoke. In 1997-98,
approximately 205 million packs of cigarettes were consumed in West Virginia.
Most people who use tobacco begin as children. Because they start young, they have more difficulty quitting and are more likely to develop a tobacco-related disease. To be effective, prevention and cessation programs need to be carefully adapted to the unique cultural, political, and economic features of West Virginia.
OBJECTIVE 27.2. Reduce the prevalence of cigarette smoking among pregnant women to 12% or lower. (Baseline: 25.4% in 1998)
Data Source: WVBPH, OEHP, Health Statistics Center (HSC)
OBJECTIVE 27.3. Increase smoking cessation during pregnancy, so that at least 60% of women who are cigarette smokers at the time they become pregnant quit smoking early in the pregnancy and maintain abstinence for the remainder of their pregnancy, following delivery, and through postpartum. (Baseline: 14.3% in 1998)
Data Source: WVBPH, Office of Maternal, Child & Family Health (OMCFH), Pregnancy Risk Assessment Monitoring System (PRAMS)
Approximately 30% of births in West Virginia are to mothers with one or more pregnancy risk factors, such as cigarettes, alcohol, or other drug use. There is a 66% greater rate of smoking among pregnant women in West Virginia than the rest of the U.S. According to West Virginia vital statistics for 1998, 12.3% of premature births occurred to mothers who smoked.
Many studies have shown that babies who are born to mothers who smoke heavily during their pregnancy are born smaller than they would have been had their mothers not smoked. A recent CDC study found that IQs were lower in the babies born to mothers who smoked than a comparable group of babies with non-smoking mothers.
According to a 1996 report prepared by the West Virginia Department
of Health and Human Resources, the proportion of births with Medicaid
coverage in West Virginia in 1993 was about 42%, a considerable increase
from the 1989 proportion of about 32%. Women with Medicaid coverage were
1.5 to 2 times more likely to smoke during pregnancy than were women without
Medicaid coverage. Average annual costs to Medicaid services to all West
Virginia women who smoke during pregnancy were estimated to be $648,978.
The estimated medical cost (Medicaid and non-Medicaid) of a complicated
birth for smokers ($10,894) was nearly twice that of nonsmokers ($6,544).
To combat the epidemic of smoking during and after pregnancy, the Tobacco
Prevention Program should continue its collaborative efforts with programs
that specifically address pregnancy to implement programs reaching this
population. Research studies must be magnified to evaluate the use of
pharmacological cessation aids for pregnant women.
OBJECTIVE 27.4. Increase to at least 80% the proportion of health care providers who routinely advise cessation and provide assistance and follow-up and document charts for all their tobacco-using patients (providers to include physicians, dentists, nurses, dental hygienists, mental health professionals, social workers, psychologists, pharmacists, medical assistants, physician assistants, and home health care aides). (Baseline data available in 2000)
Data Sources: WVBPH, OEHP, BRFSS; WV Chapter of the American Academy of Family Physicians (WVAAFP), and/or WV State Medical Association (WVSMA) surveys
OBJECTIVE 27.5. Increase to 90% the number of physicians (notably pediatricians) who advise parents not to smoke in the home around children. (Baseline data available in 2000)
Data Sources: WVAAFP and/or WVSMA surveys
In addition to ETS exposure, there are several safety reasons why cigarettes should not be in the home. Also, adult smokers provide the tobacco role model, making it twice as likely that these children will become tobacco users in adolescence and beyond.
In order to be successful in helping persons to stop smoking and decrease smoking around children, West Virginia will strive to increase the availability of cessation programming, train providers in effective cessation services, increase the availability of self-help and educational materials, and conduct campaigns to promote smoke-free homes.
OBJECTIVE 27.6. Increase to 80% the proportion of health plans that offer treatment of nicotine addiction (e.g., tobacco use cessation counseling by health care providers, tobacco use cessation programs, prescriptions for nicotine replacement therapy (NRT)/pharmaceuticals, and other cessation services). (Baseline data available in 2000)
Data Source: WVBPH, OEHP, Tobacco Prevention Program
Statistics indicate that about 50% of current adult smokers have tried to quit smoking for at least one day, but we know that their attempts may not result in success. For this population, the provision of cessation and treatment services is critical.
Health-care professionals can play an important role in cessation; however, fewer than 25% of physicians report receiving adequate training to help their patients quit smoking. Research demonstrates that even brief advice from health care providers to stop smoking is effective. More intensive interventions that provide social support and training in problem-solving skills are even more effective. FDA-approved pharmacotherapy can also help people quit smoking, particularly when combined with counseling and other interventions.
In planning for the future, health care plans, health care providers, and their consumers must be educated to the benefits of cessation services, so that cessation is viewed as basic care. West Virginia's Medicaid program and Public Employees Insurance Agency currently provide these services, and evaluation of the success of and challenges met by these programs will provide valuable information for implementation of cessation coverage in other health plans.
OBJECTIVE 27.7. Reduce smokeless tobacco use among adult men aged 18+ to 13% or lower. (Baseline: 18% in 1998)
Data Source: WVBPH, OEHP, BRFSS
According to the 1999 YRBS, 28.6% of male high school students have used chewing tobacco or snuff on one or more of the 30 days prior to their interview. Smokeless tobacco is just as addictive as cigarettes. There is nicotine in all smokeless products, but smokeless tobacco contains more nicotine than cigarettes. For example, holding an average size dip or chew in your mouth for 30 minutes gives you as much nicotine as smoking four cigarettes. Smokeless tobacco and the nicotine in it can cause all the heart and blood vessel problems that smoking causes -- higher blood pressure, reduced circulation, and faster heart rate.
OBJECTIVE 27.8. Reduce the proportion of young men in grades 9-12 who report smokeless tobacco use to 16% or lower. (Baseline: 28.6% in 1999; baseline data available in 2000 for grades 6-8)
Data Source: WVDOE, OHS, YTS and YRBS
OBJECTIVE 27.9. Increase state excise taxes on cigarettes so state excise tax is at least 30% of retail price.
Data Source: Retail sales data, WV Division of Tax and Revenue
OBJECTIVE 27.10. Increase state excise taxes on non-cigarette tobacco products so state excise tax is at least 25% of retail price.
Data Source: Retail sales data, WV Division of Tax and Revenue
The single most effective measure that can reduce youth consumption of tobacco products is to increase the price. "Price elasticity" models for cigarette consumption and sales indicate that for every 10% increase in price consumption among youth will decline by up to 14%. Price increases can be achieved by retailers increasing prices or by excise taxes, which then generate revenue for state government.
OBJECTIVE 27.11. (Developmental) Increase smoking cessation attempts among adolescent smokers. (Baseline data available in 2000)
Data Source: WVDOE, OHS, YTS
Education programs should not just focus on preventing children from starting to use tobacco, but should also address quitting for those who have already begun. Research in developing the N.O.T. (Not On Tobacco) cessation program for youth revealed that most teens who smoke say that they would like to quit, but that they cannot do it on their own. About 24% of high school students indicated that they are daily smokers (possibly experiencing nicotine dependence) and about 38% of current high school smokers have tried to quit.
OBJECTIVE 27.12. (Developmental) Increase the level of compliance and enforcement with WV Board of Education policy prohibiting tobacco use by anyone at any time on public school property to a level of no more than one incident per week reported at each school.
Data Source: WVDOE, Office of Safe and Drug-Free Schools.
West Virginia is among the leaders in states implementing these strong policies that further emphasize the "tobacco-free" norm and compliance with state law. Enforcement of such policies has been the challenge, and we are investigating a variety of solutions, including signage, volunteer monitors, student monitors and detectors/warning systems.
OBJECTIVE 27.13. Enforce state and federal laws that prohibit tobacco sales to minors to 10% noncompliance or less.
Data Source: Synar monitoring data; tobacco retailer inspection programs.
OBJECTIVE 27.14. Enact state or local laws requiring licensure of tobacco retailers, behind-the-counter displays, and restrictions on advertising, violations that may result in revocation of license.
In March 2000, the U.S. Supreme Court declared that the FDA has no authority to restrict tobacco sales and marketing, and as a result the tobacco retailer inspection program that began in April 1999 in West Virginia was immediately dissolved. This program, plus Synar monitoring data, had indicated that illegal sales to minors occurred during about 34% of attempts.
The creation of a comprehensive inspection program, including retailer education and subsequent fines and the threat of license suspension/revocation, would increase compliance with the state law and federal regulations.
OBJECTIVE 27.15. (Developmental) Increase to 95% the percentage of 6th grade students who associate harm with tobacco use; ensure that comprehensive tobacco prevention curricula are taught in public schools. (Baseline data available in 2000)
Data Source: WVDOE, OHS, YTS
In 1999, 33.7% of students surveyed in the YRBS reported that they had smoked their first cigarette before their thirteenth birthday. The CDC recommends implementing and incorporating evidence-based curricula, linking school-based efforts with local community coalitions and statewide counter-advertising programs, and implementing CDC's Guidelines for School Health Programs to Prevent Tobacco Use and Addiction, including tobacco-free policies, teacher training, parental involvement, and cessation services.
In 1999, the West Virginia Department of Education implemented Life Skills Training (identified by CDC as Programs That Work) in sixth grade and will add seventh grade in the year 2000. Life Skills Training is a research based curriculum that has been shown to significantly decrease tobacco use rates among participants. The Department of Education plans to continue the use of this curriculum.
OBJECTIVE 27.16. Increase to 85% the number of employers having 10 or more employees who have written and enforced tobacco restriction policies for the work place, designed to protect workers from exposure to ETS.
Data Source: West Virginia University, Office of Health Services Research.
Both common sense and scientific research indicate that smoking restriction policies at the work place result in fewer opportunities to smoke and more smokers quitting, but their main purpose is to protect the nonsmokers from exposure to ETS. Smokers use sick leave about 50% more than nonsmokers, and cost employers up to $1,300/year.
Most of the clean indoor air regulations require that businesses implement policies to protect nonsmokers from this exposure, but we need to encourage employers to expand the polices to create smoke-free buildings, to include smokeless tobacco use in restrictions, and to promote cessation. Baseline data on current policies and technical assistance needs will be gathered in FY2001. Trained consultants may be available later to provide technical assistance to businesses.
OBJECTIVE 27.17. Increase the number of counties covered by Clean Indoor Air (CIA) regulations; increase the level of protection from ETS for existing CIA regulations; defeat CIA preemption measures in state legislature.
Data Source: WVBPH/OEHP, Tobacco Prevention Program
By far, one policy area in which West Virginia has received critical acclaim is the adoption of CIA regulations through local boards of health. West Virginia received the 1997 Clean Indoor Air Award from Americans for Nonsmokers Rights for being the state to enact the most regulations in that year.
Of the current local CIA regulations, there is great variability in their coverage. Restaurant coverage varies from 25%+ seating for nonsmoking sections to 100% smoke-free. Business coverage is fairly consistent, priority consideration given to protecting the nonsmoker from ETS exposure. Public places (government buildings, sports and entertainment facilities, malls, etc.) vary from designated smoking areas to 100% smoke-free, and some regulations include exemptions for certain facilities. To date, CIA regulations have been adopted by 43 of the 55 counties.
Our goal moving toward 2010 is to increase the number of counties covered by CIA regulations and to increase the strength and breadth for those with existing regulations.
OBJECTIVE 27.18. Establish a statewide evidence-based comprehensive tobacco prevention and control program for West Virginia, funded by state funds to at least CDC-recommended minimum levels ($14 million per year) with sustained funding for at least five consecutive years.
Data Source: WVBPH, OEHP, Tobacco Prevention Program
Meeting the Objectives
Health Promotion Channels for Achieving Objectives:
- Worksites
- Schools
- Public Health Programs
- Networks
- Health Care System
- Higher Education
The Tobacco Prevention Program was started in West Virginia in 1991 and funded through 1998 by the ASSIST Project of NCI, with national partnership from the American Cancer Society. Since 1998, funding has come from the CDC's National Tobacco Control Program. Both federal programs provided funding between $800,000 to $1,100,000 annually and during those years, no state funds were ever allocated to this issue.
With the November 1998 signing of the tobacco settlement, West Virginia stands to receive about $60 million average per year. In accordance with WV Code §4-11A, passed in 1999, half of the funds received must go into a trust fund (which cannot be spent). The other half can be spent in several ways (PEIA programs, Medicaid, health programs and facilities). It is the goal of the WVBPH to see that CDC-recommended funding levels of $14 million to $35 million are allocated to the Tobacco Prevention Program and that decision-makers commit these funds for many consecutive years to address this public health crisis.
Some of the organizations that will be leading the initiatives to reach the objectives include:
- West Virginia Tobacco Prevention Program, Health Promotion Division, Office of Epidemiology and Health Promotion, WVBPH
- Health Statistics Center, Office of Epidemiology and Health Promotion, WVBPH
- WV Office of Maternal, Child & Family Health, WVBPH
- Coalition for a Tobacco-Free WV (CTFWV)
- WV Youth Tobacco Prevention Campaign, Healthcare Education Foundation of WV
- Office of Healthy Schools, DOE
- Division on Safe and Drug-free Schools, DOE
- WV Division on Alcoholism and Drug Abuse, OBHS
The following is a partial list of member agencies represented by the CTFWV:
- American Cancer Society, Mid-Atlantic Division
- American Heart Association, Ohio Valley Affiliate
- American Lung Association of West Virginia
- West Virginia State Medical Association
- American Academy of Family Physicians, WV Chapter
- American Association of Retired Persons
- WV Hospital Association
- WVU School of Dentistry
- WV Coalition for Minority Health
- WVU Prevention Research Center
- March of Dimes Birth Defects Foundation, WV State Chapter
- Wellness Council of West Virginia
Work Group Members
Kathi Elkins, Work Group Leader, Policy and Planning Specialist,
WV Tobacco Prevention Program, WVBPH
Christina Mullins, Associate Program Director, WV Tobacco Prevention
Program, WVBPH
Amy Thomas, Program Coordinator, WV Tobacco Prevention Program,
WVBHP
Cinny Kittle, Project Director, WV Youth Tobacco Prevention Campaign
Debra Southerland, former coordinator, Coalition for a Tobacco-Free
WV
Chantal Centofanti-Fields, Director, Programs and Services, American
Lung Association of WV
Hersha Arnold, Cancer Control Manager, American Cancer Society
J. Dean Lee, Coordinator, Office of Healthy Schools, WVDOE
Robert H. Anderson, PhD, Prevention Research Center, WVU
Norm Streenstra, Executive Director, Citizens Action Group
Madrith Chambers, WV Minority Health Coalition
Stanley Mills, Sanitarian, Cabell County Health Department
Sandria Glasscock, Grant County Health Department
Gus Nelson, former Tobacco Education Coordinator, Mid-Ohio Valley
Health Department
Jill Rosenthal, former Program Manager, Center for Rural Health
Development
Susan Anderson, WV Health Promotion Specialist, Region VI
Daniel Foster, MD, former Chair, 1998-2000,
Coalition for a Tobacco-Free WV
Jacquelynn Copenhaver, Rivers and Bridges Consortium
Sidney A. Rosenbluth, PhD, MS, BS, Department of Pharmaceutical
Systems & Policy
Anna Reno, RHEP Site Coordinator, Little Kanawha Area Consortium
References/Resources
U.S. Bureau of the Census. 1997 Census Data. Washington, DC: 1998.
Agency for Healthcare Research and Quality. Treating Tobacco Use and Dependence: A Clinical Practice Guideline. Washington, DC: U.S. Department of Health and Human Services, 2000.
American Cancer Society. What Tobacco Costs America. Atlanta, GA: ACS, April 1997.
California Environmental Protection Agency. Health Effects of Exposure to Environmental Tobacco Smoke. Sacramento, CA: Office of Environmental Health Hazard Assessment, September 1997.
CDC. Best Practices for Comprehensive Tobacco Control Programs. Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service, August 1999.
CDC. State Tobacco Control Highlights 1999. CDC Publication No. 099-5621, pgs. 106-107. Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service, 2000.
National Institutes of Health. Cigars: Health Effects and Trends,
1998. Monograph 9, Chapter 4. Washington, DC: U.S. Department of Health
and Human Services, February 1998.
Dye TD. Medicaid Coverage for Pregnant Women and Infants: Outcomes,
Costs, and Opportunities. Charleston, WV: West Virginia Department
of Health and Human Resources, 1996.
Eden A. ParenTalk Newsletter. National Parenting Center, Oct. 24, 1995. www.tnpc.com/parentalk/pregnancy/preg49.html
Fiscal Year 2000-2001 Budget. Charleston, WV: West Virginia Department of Health and Human Resources.
CDC. Health Consequences of Using Smokeless Tobacco. Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service, 1996.
Kristein M. "How much can business expect to profit from smoking cessation?" Preventive Medicine 2:358-381(1983).
National Association of Attorneys General. Documents pursuant to the multi-state settlement agreement. www.naag.org. November 1998.
National Cancer Institute. Cigarettes, Chewing Tobacco and Snuff: State Excise Tax Laws. State Cancer Legislative Database Program: August 1999.
Satcher D. Washington Post, September 6, 2000, p. A19.
Report to Congress for 1996 Pursuant to the Federal Cigarette Labeling and Advertising Act (1998).
Coalition for a Tobacco-Free West Virginia. Saving Lives and Saving Money: Blueprint for a Comprehensive Tobacco Prevention Program for West Virginia. Charleston, WV: CTFWV, November 1999.
Schoendorf KC and Kiely JL. "Relationship of sudden infant death syndrome to maternal smoking during and after pregnancy." Pediatrics 90:905-908 (1992).
National Cancer Institute. The Health Effects of Exposure to Environmental Tobacco Smoke: the Report of the California Environmental Protection Agency. Smoking and Tobacco Control Monograph 10. Washington, DC: U.S. Department of Health and Human Services, 1997.
Tobacco Fact Sheet. 11th World Conference on Tobacco OR Health, Summer 2000.
Tobacco Institute. The Tax Burden on Tobacco. Historical Compilation, Vol. 28, Exh. 9 to Adams deposition, 1997.
CDC. "Advances in the knowledge of the health consequences of smoking." U. S. Surgeon General's Report, 1989. Chapter 2. Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service,.
WV Bureau for Public Health. The Effect of the Tobacco Excise Tax Act on the Prevalence of Cigarette Smoking in the State of West Virginia. Charleston, WV: West Virginia Department of Health and Human Resources, 1998.
WV Bureau for Public Health. Synar Monitoring: 1999 Provisional Results of Random Unannounced Inspections of Tobacco Outlets in West Virginia. Charleston, WV: West Virginia Department of Health and Human Resources, 1999.
WV Bureau for Public Health. West
Virginia County Health Profiles, 2000. Charleston, WV: West Virginia
Department of Health and Human Resources, 2000.
WV Bureau for Public Health. West Virginia Vital Statistics 1998. Charleston, WV: West Virginia Department of Health and Human Resources, 1998.
Office of Healthy Schools. 1999 Youth Risk Behavior Survey. Charleston, WV: West Virginia Department of Education, 1999.
WV Bureau for Public Health. Behavioral Risk Factor Survey 1998. Charleston, WV: West Virginia Department of Health and Human Resources, 1999.
WV Bureau for Public Health. Tobacco Is Killing (and Costing) Us, Charleston, WV: West Virginia Department of Health and Human Resources, 1999.
For More Information
Tobacco Prevention Program
Office of Epidemiology and Health Promotion
350 Capitol Street, Room 319
Charleston, WV 25301-3715
Phone: (304) 558-0644; Fax: (304) 558-1553
This page was last updated June 28, 2001.
For additional information about HP2010, contact Chuck Thayer at (304) 558-0644
or Chuck.E.Thayer@wv.gov