Contents
| WV | DHHR | BPH | OCHSHP | HSC |
Obesity:
Facts, Figures, Guidelines
Section Three
THE PUBLIC HEALTH APPROACH TO ADDRESSING OBESITY
Introduction. The Flagship Objective for the Nutrition and Overweight West Virginia Healthy People 2010 Objectives states, “Reduce the proportion of people aged 18 and older who are obese.” In order for this objective to be met, other related West Virginia Healthy People 2010 Objectives must also be addressed, for example, the Flagship Objective for Physical Activity and Fitness, “Reduce to 37% the proportion of people aged 18 and older who engage in no leisure-time physical activity.” Meeting these objectives would make a great difference in the prevention and control of chronic diseases in West Virginia. Many other objectives relate to increasing physical activity and increasing healthy eating as well; these can be found in Appendix B, in A Healthier Future for West Virginia: Healthy People 2010 (96), or accessed on the Internet at www.healthywv.org.
Obesity is multifactorial, as explained in Section One of this document; thus, addressing the burden of obesity cannot be a singular effort. It will take many programs working in collaboration to fully address and intervene effectively upon the behaviors of physical activity and healthy eating. Instituting policy and environment changes enables public health to use a population-based approach to behavior change. The key to this approach is using public health’s strength to bring partners to the table to plan and intervene using available resources. As resources are not always abundant, it is important to use existing programs to begin to address these issues. This can be accomplished by using a “best practices model” for addressing chronic disease in general.
BEST PRACTICES MODEL FOR ADDRESSING CHRONIC DISEASE
Practices and Programs That
- focus on the elimination of disparities
- are affordable and sustainable
- are population based
- are science-based and effective
- are replicable and relatively easy to implement
- are well-defined with clear goals and measurable objectives
- are valued by stakeholders
- are comprehensive and inclusive
- are acceptable to the target population
- are accessible and
- focus on growing communities and building social capital
Examples of addressing the problem of obesity with already existing chronic disease program efforts can include:
1. Continuing to obtain obesity measures (height/weight and/or BMI) while assessing diabetes and/or cardiovascular disease quality indicators: HgA1c, blood pressure, cholesterol, etc.
2. Using existing professional networks such as the cancer information specialists to counsel on increasing physical activity and healthy eating patterns.
3. Using cardiovascular health programs to promote physical activity and healthy eating initiatives with a special emphasis on disparate populations.
The best practices model allows agencies and programs to assess where
resources are already in place and working. Partners can see the bigger
picture and make wise decisions to assure that, as gaps are identified,
new resources can be focused on those areas, thus avoiding duplication
of resources and efforts.
Working with community health promotion programs is critical to the success
of a comprehensive effort. While broad, overarching state-level interventions
are necessary, just as important are the interventions at the local level.
Coalition building and work at the grassroots level can produce bottom-up
support at the same time top-down efforts are being pursued. It will take
all components of a chronic disease and community health promotion program
to prevent, treat, and control obesity.
A strong physical activity and nutrition strategic plan must be developed and incorporated by all chronic disease programs. Each program should select an area of focus; these areas then form the basis for the overall plan. Once roles between the programs are identified and resources allocated appropriately, a comprehensive effort can be attained.
Comprehensive Nutrition and Physical Activity Program. In 2002, the Nutrition and Physical Activity Workgroup (NUPAWG), in collaboration with the Centers for Disease Control and Prevention, released a report entitled Guidelines for Comprehensive Programs to Promote Healthy Eating and Physical Activity (97).13 According to the NUPAWG, the goals of a Comprehensive Nutrition and Physical Activity Program are to:
- Promote healthy eating that follows national dietary guidance policy.
- Maintain recommended levels of moderate and vigorous physical activity from childhood through adolescence into adulthood.
- Eliminate disparities in diet, physical activity, and overweight among disadvantaged population groups.
- Increase access to healthy foods and to opportunities to be active for every age and population group.
- Promote healthy weight among adults and children.
Obesity Prevention Program. The West Virginia Bureau for Public Health will use these guidelines in the development and implementation of a comprehensive nutrition and physical activity program, or an Obesity Prevention Program, which will include the following seven components. The best practices model shown on page 45 will drive the planning for the program. The Bureau will coordinate all current chronic disease programs in a collaborative fashion while directing new funds and resources toward a fully comprehensive program. In this way, West Virginia can address most or all of the Healthy People 2010 Objectives related to obesity.
1. Leadership, Planning/Management, and Coordination
Each state needs the capacity to frame the issues, create a vision, set goals and objectives, determine strengths, and integrate a comprehensive set of intervention programs. Along with the visionary elements comes the crucial need to develop infrastructure and attract resources.
The West Virginia Coalition for Physical Activity and the West Virginia Nutrition and Chronic Disease Coalition were both established in the early 1990s to address the state’s Healthy People 2000 and 2010 objectives. Both are facilitated by WVBPH’s Cardiovascular Health Program, which drew together many agencies and individuals to (1) select the WV Healthy People 2010 Objectives and (2) subsequently develop strategies to meet these objectives.
The WV Coalition for Physical Activity has several state and local level representatives from higher education, WV Department of Transportation, WV Division of Tourism, WV Trails Coalition, school health, and nonprofit associations among its membership. The coalition’s efforts currently center on creating walkable communities and increasing opportunities for youth to be more active during school hours. The WV Coalition for Physical Activity will continue to address the issues of obesity prevention as they relate to physical activity.
The WV Nutrition and Chronic Disease Coalition membership includes representatives from the Public Employees Insurance Agency, Highland Hospital, West Virginia University, WVBPH’s Office of Nutrition Services, WV Coalition on Food and Nutrition, American Cancer Society, and WV Dairy Council, among others. Its current priority areas address the USDA’s 5-A-Day program to increase consumption of fruit and vegetables and healthy portion sizes. The WV Nutrition and Chronic Disease Coalition will continue to focus on the issues of obesity prevention relating to nutrition.
Priority populations for the Obesity Prevention Program were identified
based on data from The Burden of Cardiovascular Disease in West Virginia,
a 2001 report issued by the WV Bureau for Public Health (98). These populations
are underserved youth, seniors, racial and ethnic minorities, and women
18 to 34 years of age.
The physical activity, nutrition, and priority populations coordinators,
all located within the WVBPH’s Division of Health Promotion and
Chronic Disease, are organizing efforts in their specific areas within
existing chronic disease programs. The coordinators work through the Bureau’s
internal programs and with other outside agencies, organizations, and
community members to best determine how to improve physical activity and
nutrition by using policy and environment approaches.
2. Environmental, Systems, & Policy Change
Interventions aimed at the individual are by themselves insufficient to modify and sustain healthy behavior. Environments that support, facilitate, and even require healthy behaviors are necessary for large-scale, long-term change. Passive public health interventions (i.e., policies that alter the food supply or the physical activity environment) yield greater and more sustainable changes in larger populations.
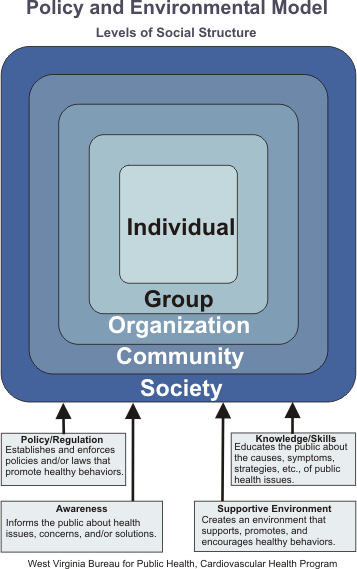
Policy interventions refer to laws, regulations, and rules, both formal and informal, that determine what is socially acceptable behavior, e.g., clean indoor air ordinances. Environmental interventions include changes to the economic, social, or physical environment in which people live, work, and play. Examples of these include offering different, and healthier, choices in vending machines and making stairways as safe and easily located as elevators. Policy and environmental change tends to fall into one or more of four categories: (1) availability or accessibility of consumer products; (2) physical structures or physical characteristics of products; (3) social structures and policies, or (4) cultural and media messages.
Representatives from several state agencies and legislators participated in the National Governors’ Association Policy Academy, where state policy initiatives such as removing the tax on produce (fruits and vegetables), implementing daily physical activity during the school day, and updating nutrition standards in senior centers were addressed.
An inventory of environmental and policy changes is being compiled by
the WVBPH. Community tool kits (including assessment surveys) are under
development, and community groups will be trained on how to implement
policy and environmental changes at the local level. The tool kit will
be piloted with priority population groups.
3. Mass Communication
Mass media interventions reach all members of society and unify social action to drive consumer demand for healthy behaviors in the marketplace. They support community programs, raise visibility, and help sustain behavior change.
The WVBPH partially supported the Wheeling Walks Campaign in collaboration with West Virginia University and the Wheeling-Ohio Health Department. The intensive media-based community physical activity campaign used paid advertising, public relations, and community educational activities to deliver a targeted public health message: the promotion of 30 minutes or more of moderate-intensity walking almost every day. The model is being transformed into a training model/CD ROM for statewide distribution.
The WVBPH also partially supported the 1% or Less Campaign in Clarksburg, WV. This campaign, which attracted national attention, more than doubled the community’s low-fat milk consumption, from 18% to 41% of milk sales.
There is much that can be learned from the above two campaigns in terms of cost effectiveness and replicability. The Bureau’s Division of Tobacco Prevention has also used counter marketing and media advocacy efforts in its programs. Adapting these methods to promote healthy eating and physical activity must be a priority.
4. Community Infrastructure & Programs
The social, physical, cultural, and political environments in communities affect knowledge, beliefs, attitudes, and behaviors related to prevention. Community-based interventions should involve members in creating environments where healthy choices are easy choices and help develop social capital and sustainable economies.
The state-supported Community-Based Initiatives Grants Program funds community projects that address the West Virginia Healthy People 2010 Objectives for Physical Activity and Fitness and Nutrition and Overweight by using policy and environment strategies. Funding priority is also given when priority populations are targeted. This program, in conjunction with the regional Health Promotion Specialists Network, has helped build the infrastructure necessary for successful community-based programs.
Regional and/or county health networks can be mobilized to address obesity prevention in a collaborative fashion. Many of these networks are already established, including the Adolescent Health Initiative, the cancer information specialists, and the WVU Extension Service. Involving nontraditional partners such as city councils, regional planning development councils, and economic development agencies can build on these efforts.
5. Programs for Children & Youth
Young people need to build healthy bodies and establish healthy lifestyles. Yet the school environment is less supportive of health and has less access to healthful choices than ever before. The WVBPH has partnered with the WV Department of Education’s Office of Healthy Schools to address the WV Healthy People 2010 Objectives. Collaborative projects have included collecting data to establish baselines, completing inventories, developing Walk to School initiatives, and training principals.
Several other youth programs are currently being implemented, such as Coronary Artery Reduction and Detection In Appalachian Communities (CARDIAC), Healthy Hearts Internet Module, Helping Educators Attack CVD Risk Factors Together (HEART), and Choosy Kids. (Program descriptions are provided in Appendix C.) School and community-based programs are vital to the improvement of youth behaviors in physical activity and nutrition.
6. Health Care Delivery
Health care delivery systems can play an important role in promoting chronic disease prevention. This may involve setting up office-based systems for anticipatory guidance and non-pharmacologic disease management that includes screening, assessment, counseling, and referral for treatment, along with incentives for leading a healthy lifestyle.
Chronic disease programs are addressing obesity prevention through the assessment of BMI and other clinical indicators through compliance to provider protocols. Obesity prevention can be addressed by the health care delivery system through such strategies as provider training, linking providers to community physical activity and healthy eating programs, working with third party payors for reimbursement for counseling and referrals, the implementation of disease management programs, etc. It will take many agencies and associations working together to accomplish these efforts.
7. Surveillance, Epidemiology, and Research
This component is essential for monitoring trends, setting priorities, planning programs, mobilizing action, allocating resources, and evaluating results. A mix of survey, surveillance, and qualitative research with consumers and intermediaries is needed.
West Virginia uses the Behavioral Risk Factor Surveillance System to determine patterns of physical activity and overweight/obesity among the state’s adults. The Youth Behavioral Risk Factor Survey, which is implemented by the WV Department of Education, collects data on physical activity and dietary patterns among high school students. Additional data collected through oversampling, special surveys, and sentinel surveillance systems are necessary to determine program design, implementation, and evaluation of a comprehensive obesity prevention program.
The West Virginia Bureau for Public Health will use the NUPAWG guidelines to develop and implement its Obesity Prevention Program. Incorporating the seven components described above into this effort will allow the Bureau to involve all current chronic disease programs in the creation of a comprehensive obesity prevention program.
13The report was modeled after the 1999 Best Practices for Comprehensive Tobacco Control Programs. Return to Text