The Burden of Cardiovascular Disease in West Virginia
Credits
Summary
Chapter 1
Chapter 2
Chapter 3
Chapter 4
Chapter 5
Chapter 6
References
Appendix A
Appendix B
Appendix C
Appendix D
 Chapter One
Chapter One
Introduction to the Problem of Cardiovascular Disease
Minorities | Age | Gender
Since 1940, cardiovascular disease (CVD) has been the number one killer in both the United States and West Virginia (1). Although the nation has witnessed an overall 20% decrease in CVD deaths during the past decade, CVD remains the leading cause of death and disability among both sexes and all races, at enormous cost to all. The economic cost (i.e., health expenditures and lost productivity) of CVD in the United States in 2001 is estimated to be $298.2 billion (2).
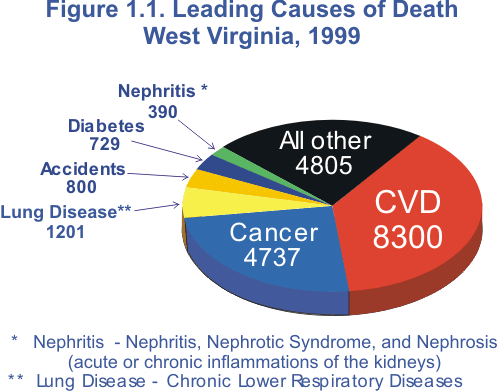
"Cardiovascular disease" refers to major disorders of the heart and the arterial circulation supplying the heart, brain, and peripheral tissues (3). Heart disease and stroke, the two main categories of cardiovascular disease, are the first and third leading causes of death, respectively, in the state and nation. Together, they accounted for 37.8% of total deaths in the United States in 1998 (the latest year for which data were available at time of publication) and 39.5% of total deaths in West Virginia in 1999.
Each year, over 1,100,000 Americans have a new or recurrent heart attack; approximately 400,000 will die (4). Coronary heart disease (CHD) accounts for approximately half of cardiovascular disease deaths and nearly one-fourth (23%) of deaths from all causes (2). CHD, also called ischemic heart disease and coronary artery disease, comprises several disorders that restrict blood flow to the heart. Cerebrovascular disease, or stroke, occurs when a blood vessel to the brain either bursts or is clogged by a blood clot, depriving the brain of oxygen and nutrients. It is frequently referred to as a "brain attack."
Clinical CVD usually manifests in middle or old age; however, atherosclerosis, the underlying process that results in CVD, begins much earlier, often as early as childhood. Atherosclerosis is the gradual build-up of plaque, or fatty deposits, on the inner walls of the arteries, causing the arteries to slowly thicken and restrict blood flow. In addition to narrowing the arteries, these plaques can rupture and form blood clots that can break off and clog a vessel leading to the heart or the brain, resulting in a heart or brain attack. Smoking, poor diet, overweight, and lack of exercise can all have an effect on the formation of plaque and are discussed later in this report. In addition, mounting evidence suggests that high homocystine levels in the blood plasma may be a factor in CVD development, as well as chronic inflammation in the blood that may activate blood-clotting mechanisms (5). Recently released results of a study by researchers with the Kaiser Permanente health plan showed that asthma sufferers (chronic lung inflammation) were 32% more likely to be hospitalized or die from heart disease than persons without asthma (6).
Top of PageCVD and Minorities. Cardiovascular disease is an equal opportunity attacker -- it strikes indiscriminately. White, black, rich, poor, educated or not, it makes no difference: CVD is a killer. Some groups, however, are disproportionately affected. African Americans are significantly more likely to die from cardiovascular disease than whites. Nationally, the heart disease death rate for African American men is 1½ times that for African American women and over twice that for their white male peers (7), while the death rate for stroke is almost twice as high for African American men as white men and 77% higher in African American women than white women (8). A study of over 10,000 urban emergency room patients found that doctors were four times more likely to miss diagnosing a heart attack in a nonwhite patient than in a white patient; quoting Pope et al. in the New England Journal Of Medicine in April 2000, "5.8% of black patients with acute myocardial infarction were not hospitalized, as compared with 1.2% of the white patients" (9). Reporting in the Journal of the American Medical Association in 2001, Stanford University researchers found that African American and Mexican American women have an increased risk of developing cardiovascular disease over white women; both overall lower socioeconomic status and cultural and/or genetic differences were found to be independently related to this risk (10).
Top of PageCVD and Age. As are most chronic illnesses, cardiovascular disease is primarily a disease of aging. It has been projected that the elderly population in the U.S. will increase by 2.6% annually after the Baby Boomers begin to turn 65 in 2010; by 2020, one in five Americans will be 60 years of age or older. "Disease Incidence and Prevalence in the US," a report published by Medical Data International, estimates a minimum increase in heart disease of 3.4% per year as a result of the graying of America (11). This fact in itself is alarming, but even more disturbing is the recent increase in heart mortality among young persons. According to the results of a study conducted by the U. S. Centers for Disease Control and Prevention (CDC), deaths from cardiac arrest 1 among persons under the age of 35 increased from 2,710 to 3,000 between 1989 and 1996. Of particular concern to researchers are the disparities unearthed by the study: the cardiac arrest death rate rose 19% among African Americans compared to 14% among whites and three times faster among young women than among young men (12). This increase parallels the increased prevalence of many of the cardiovascular disease risk factors, e.g., smoking, high cholesterol levels, and obesity, among youth as well as adults.
Top of PageCVD and Gender. One of the major misconceptions about CVD is that women have less to fear from the disease than do men, that, by and large, CVD is a man's disease. In a 1997 survey reported by the American Heart Association (13), only about 8% of the 1,000 women interviewed knew that heart disease and stroke are the greatest health threat to women. This is particularly true after menopause, at which time a woman loses the protective influence of increased estrogen levels. In 1997 CVD took the lives of over 500,000 women in the U.S., nearly twice the number of all cancers combined. More frightening still, a 1995 Gallup poll found that one-third of primary care physicians were unaware that CVD was the biggest killer of women; another survey found that 60% of primary care doctors felt themselves to be less adept at diagnosing heart disease in women than in men (14).
One reason for the erroneous belief, even among the medical community, that CVD is not as serious a problem for women as for men is that distinct gender differences exist in the development, manifestation, and treatment of, as well as mortality from, this disease. Two-thirds of those same doctors who felt uneasy over their skill in diagnosing CVD in women mistakenly believed the warning signs of the disease were the same in both sexes (14). Women have smaller hearts than men, and their arteries are finer and more fragile. These facts, plus the hormonal role that estrogen is thought to play in the disease, contribute to differences in CVD presentation. Most people are aware that a heart attack can be signaled by pressure, pain, or fullness in the chest, pain that spreads to the shoulders, neck, or arm, and/or lightheadedness, nausea, sweating, and shortness of breath. In addition, women may have other, less common, warning signs such as stomach pain, unexplained anxiety, weakness or fatigue, and/or palpitations. Even with identical symptoms, however, women are more likely to be misdiagnosed. As a result, many women don't receive the care they need until the disease has progressed significantly: 38% of women will die within one year after a heart attack compared to 25% of men (13).
It is time to assess what we know about CVD in West Virginia. We know the problem of cardiovascular disease in our state is immense; it places a huge burden on individuals, families, society, our public health system, and our limited health care resources. We know the costs of the disease are tremendous and must be addressed. We know that many factors in the development and progression of the disease are related to our lifestyles and, as such, are under our control. It is the purpose of this report to evaluate the impact of CVD on West Virginia and West Virginians, to begin to define the problem more concretely in terms of individual behavior and responsibility, the economic costs resulting from CVD-related hospitalizations and disability, and the toll taken through loss of life. Access among state residents to treatment for CVD-related diagnoses is examined in Chapter Five. Finally, Chapter Six gives an overview of the West Virginia Cardiovascular Health Program, located within the Division of Health Promotion, Office of Epidemiology and Health Promotion, West Virginia Bureau for Public Health, which is providing direction and leadership in addressing the problems of CVD in our state.
1 Unlike a heart attack, cardiac arrest is caused by a malfunction of the electrical impulses that keep the heart beating; however, the underlying disease process (altherosclerosis) remains the same.