 |
HSCStatistical BriefNumber 7April 2002 |
 |
Infant Mortality Statistics by Race
West Virginia Residents
Brief No. 7
West Virginia's infant mortality rate decreased 36% between 1980 and 1999, from 11.8 deaths of an infant under the age of one year per 1,000 live births to 7.6, as illustrated in Figure 1. Over that 20-year period, the rates have ranged from a high of 13.0 reported in 1981 to a low of 6.1 in 1994.

| Infant Mortality Rates, West Virginia Residents, 1980-1990 | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| 1980 | 1981 | 1982 | 1983 | 1984 | 1985 | 1986 | 1987 | 1988 | 1989 |
| 11.8 | 13.0 | 11.4 | 10.9 | 11.0 | 10.7 | 10.2 | 9.8 | 9.1 | 9.4 |
| 1990 | 1991 | 1992 | 1993 | 1994 | 1995 | 1996 | 1997 | 1998 | 1999 |
| 9.8 | 8.1 | 9.1 | 8.6 | 6.1 | 7.6 | 7.2 | 9.5 | 8.1 | 7.6 |
According to the Centers for Disease Control and Prevention, birthweight and period of gestation are the two most important predictors of an infant's subsequent health and survival. In addition, it is recognized that birthweight and gestational age are often factors of the mother's entry into prenatal care, and all three indicators can vary by race. For these reasons, this brief addresses infant mortality in West Virginia by race in terms of birthweight, gestational age, and prenatal care. Another HSC Statistical Brief, "Smoking: Effects on Mothers and Babies in West Virginia, Brief No. 4," examines maternal smoking and infant mortality by race. It is available through HSC by calling (304) 558-9100 or on the Center's web site at http:www.wvdhhr.org/bph/oehp/hsc/briefs/four.
Data used in this report are based on birth and death certificates filed for West Virginia residents with the State Registrar, regardless of where the event occurred. In calculating race-specific rates, numbers in the numerator are based on race of decedent, while numbers in the denominator are based on race of mother (number of infant deaths/number of live births).
Infant Mortality Rates by Race
Figure 2 depicts infant mortality rates by race for the four five-year periods between 1980 and 1999. White infant mortality rates were lower than nonwhite rates during all time periods. While rates for white infants declined steadily over the four time periods, rates for nonwhite infants dropped sharply after 1985-90, followed by a small increase in 1995-99.
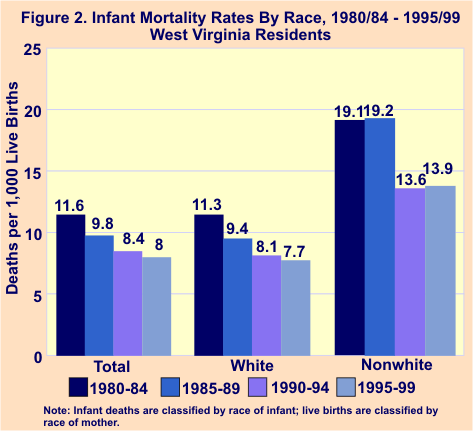
Infant Mortality and Birthweight
A line graph using a logarithmic scale to illustrate the relationship of infant mortality rates with eight birthweight categories is shown in Figure 3. As shown, infant mortality rates are exponentially higher among infants with the lowest birthweights, decreasing dramatically as birthweight increases, up to 3500-3999 grams. This scale best illustrates the fact that an infant's chances of survival increase rapidly with increased birthweight.
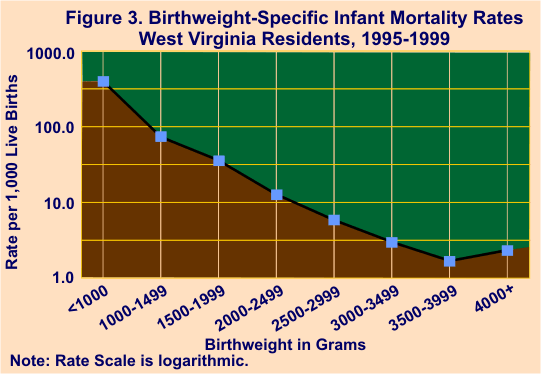
Infant Mortality and Live Births by Birthweight and Race
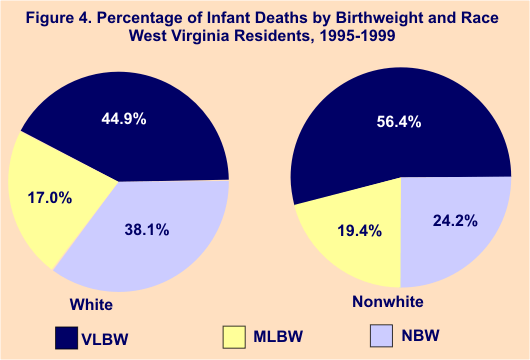
Three-quarters (75.8%) of deaths of nonwhite infants from 1995 through 1999 involved low-birthweight babies, i.e., those weighing less than 2,500 grams (5.5 pounds) at delivery. Over one-half (56.4%) were among infants with very low birthweight, less than 1,500 grams or 3.3 pounds, with 19.4% involving moderately low-birthweight infants (1,500-2,499 grams).
Sixty-two percent (61.9%) of white infant deaths during that same time period occurred among low-birthweight babies. Forty-five percent (44.9%) of white infant deaths involved babies with very low birthweight and 17.0% infants of moderate low birthweight.
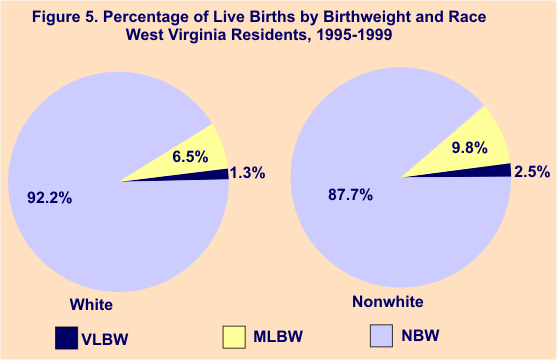
Of all births during 1995-99, a total of 12.3% of those born to nonwhite mothers were low birthweight, 9.8% moderately low birthweight and 2.5% very low birthweight. Among white mothers, a total of 7.8% of births were low birthweight, 6.5% moderately low birthweight and 1.3% very low birthweight. Figures 4 and 5 illustrate these differences.
Infant Mortality and Live Births by Gestational Age and Race
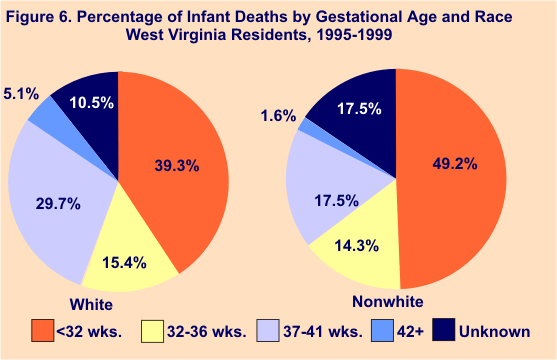
A preterm birth is defined as one occurring prior to 37 weeks of gestation. Moderately preterm infants are those born between 32-36 weeks of gestation, while very preterm infants are those born at less than 32 weeks of gestation. In the five-year period from 1995 through 1999, almost half (49.2%) of nonwhite infant deaths occurred among infants who were very preterm, while another 14.3% occurred among moderately preterm infants. Approximately four out of 10 (39.3%) white infant deaths during that time period involved very preterm infants, and 15.4% involved moderately preterm babies.
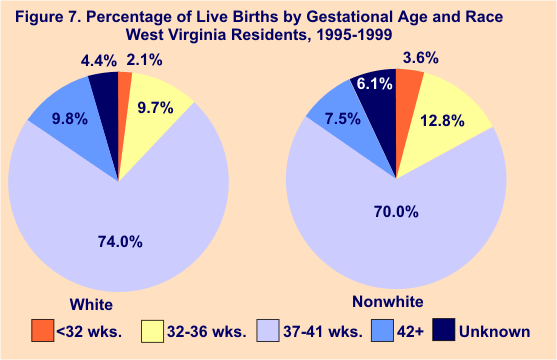
Proportionately, more births to nonwhite mothers from 1995-99 were premature than births to white mothers, 16.4% vs. 11.8%, respectively. Nonwhite mothers had higher percentages of both very preterm and moderately preterm births than did white mothers. Figures 6 and 7 illustrate the differences in infant deaths and live births by gestational age and race.
Infant Mortality and Live Births by Prenatal Care and Race
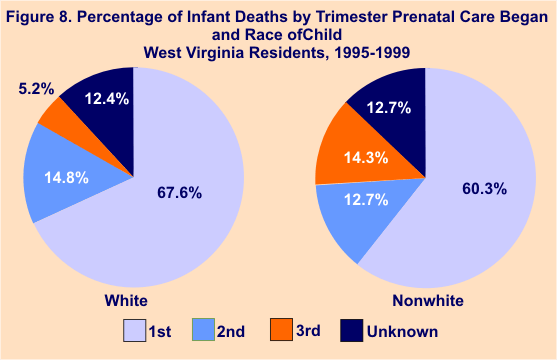
More than one in four (27.0%) deaths of nonwhite infants in West Virginia from 1995-99 involved the child of a mother who had not received prenatal care in the first trimester of her pregnancy, compared to one in five (20.0%) white infant deaths.
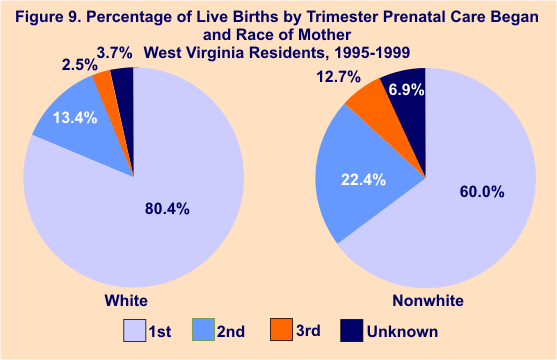
Of total births during that time period, only 65.0% of nonwhite mothers received first trimester care, compared to 80.4% of white mothers. Figures 8 and 9 illustrate the differences in prenatal care received by race for infant deaths and live births.
Conclusion
Infant mortality continues to occur more frequently among nonwhite infants than among white infants. Birthweight and gestational age are two of the most significant predictors of an infant's survival. A higher percentage of births to nonwhite mothers result in low-birthweight infants, and a higher proportion of nonwhite infants deaths occur among infants of low birthweight. Similar racial disparities are reflected in data on births and deaths of preterm infants.
Early entry into prenatal care is recognized as crucial to a healthy
pregnancy outcome, decreasing the chances of preterm and/or low-birthweight
births. Higher percentages of nonwhite mothers than white mothers did
not receive first trimester prenatal care from 1995-99, and a higher percentage
of deaths of nonwhite infants than deaths of white infants during those
years involved infants whose mothers reported late or no prenatal care.
The reasons for the disparity in infant mortality between white and nonwhite
infants are many and complex; however, the decreased likelihood of first
trimester care among nonwhite mothers, in turn yielding a greater likelihood
of low-birthweight and/or preterm births, must be addressed as a contributory
factor to the increased mortality among nonwhite infants.